VTE Intervention

Venous thromboembolism (VTE) — includes deep vein thrombosis (DVT) and pulmonary embolism (PE) — affects 1 out every 1000 inpatients in the US and is the second leading cause of medical complications resulting in lengthening hospital stays.1,2 Annual VTE-related deaths for the USA estimates at 296,000 and 370,000 for Europe.3
With an annual cost of USD 27.2 billion on treating initial hospital-acquired VTE events (52% as hospital-acquired preventable costs) and another USD 34.4 billion for hospital-acquired VTE reoccurrence treatments (56% as hospital-acquired preventable costs), VTE-related hospital expenses impose a heavy burden on healthcare systems.4
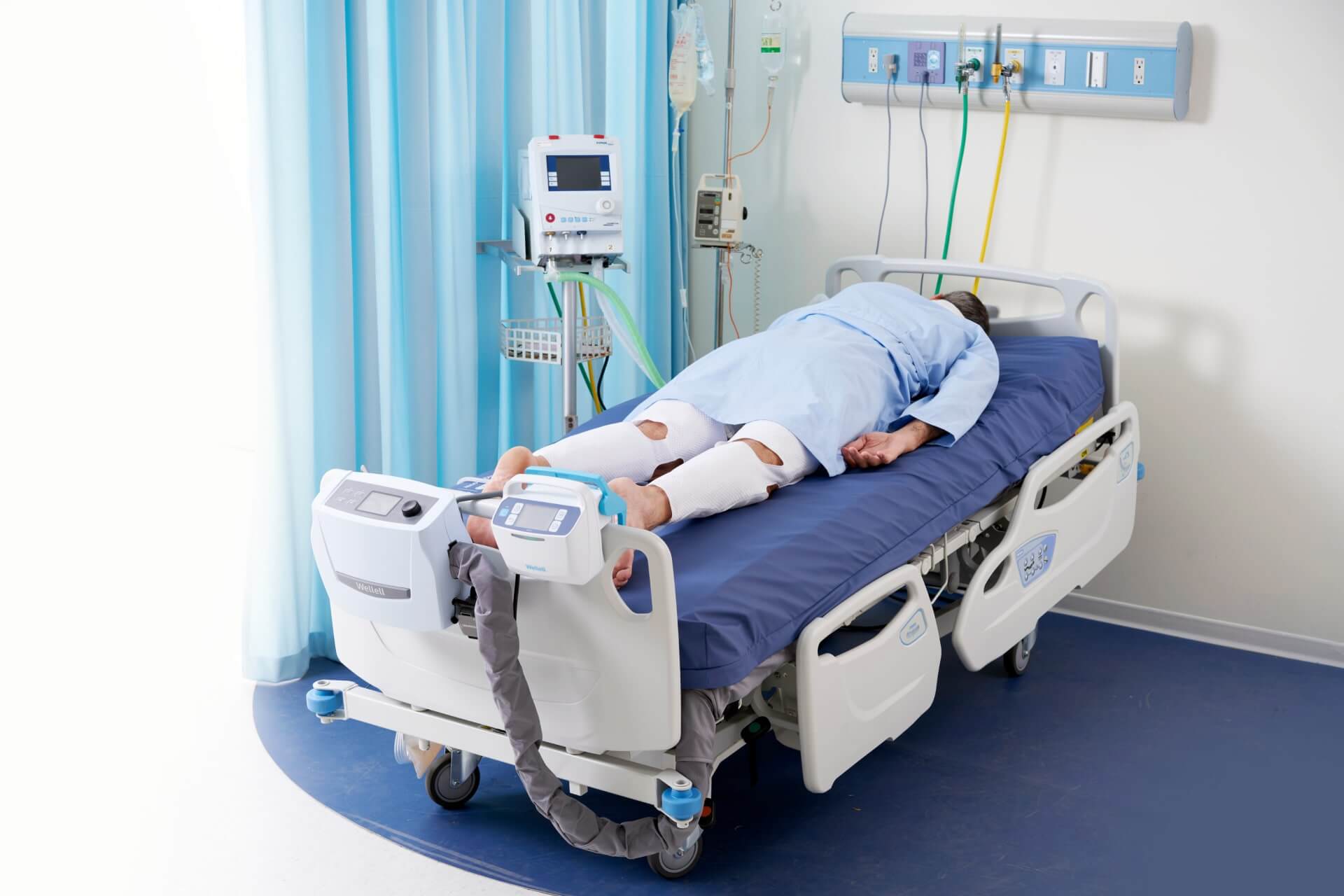
Intervention reduces DVT incidences by 70%.
Every year, US healthcare treats over 600,000 VTE incidences1, most commonly for the lower extremities.5,6
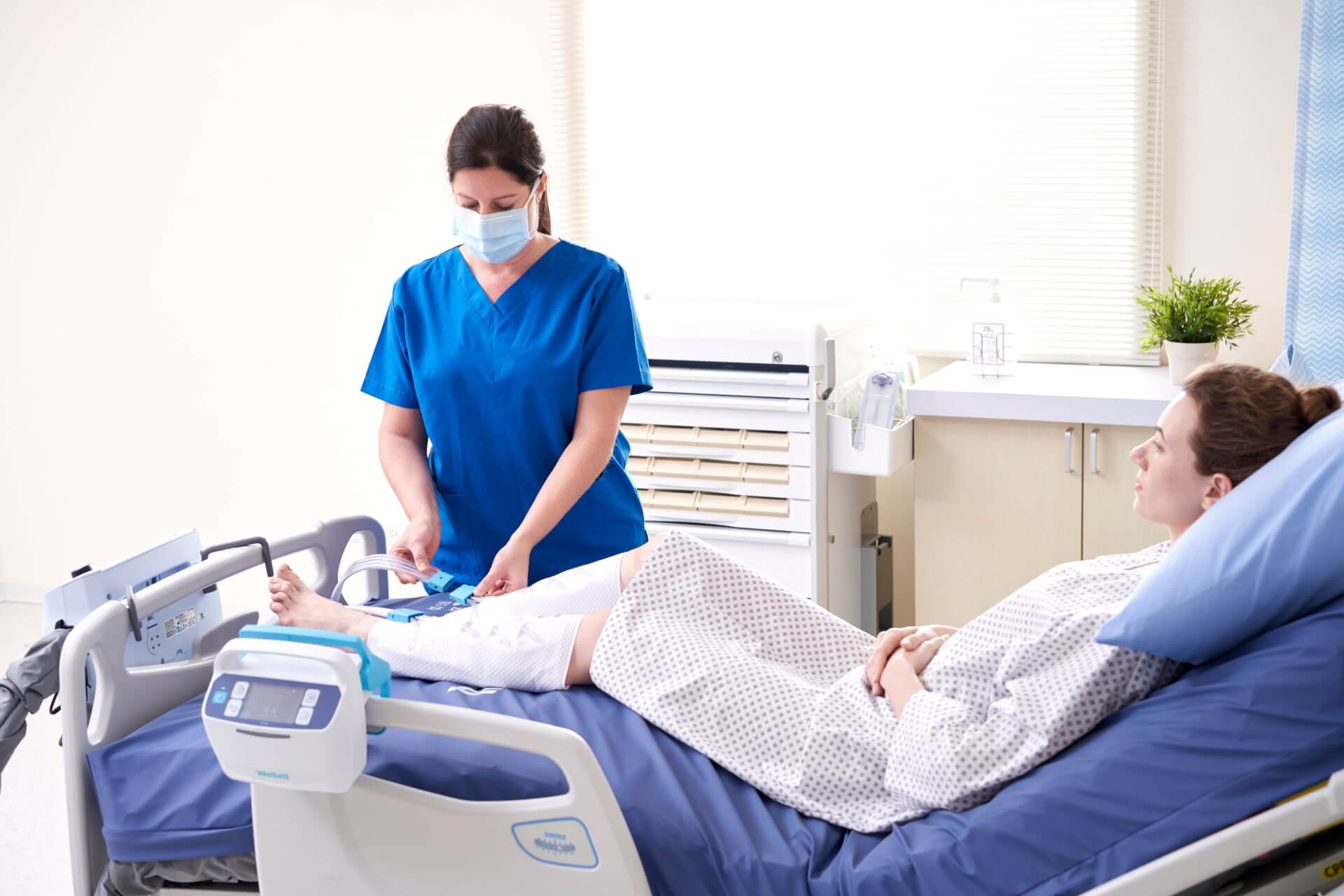
1 out of every 1000 inpatients develop DVT every year (US)
American College of Chest Physicians® recommends mechanical VTE intervention for hospitalized acutely and critically ill inpatients at a high risk of major bleeding. Effective VTE interventions significantly reduce costs, risk of reoccurrences, morbidity, and mortality.7

DVT complications increase length of stay by 9 days.
20% to 50% of patients with proximal DVT develop post-thrombotic syndrome (PTS), and 5% to 10% progress into severe cases such as venous ulcers , which increases the length of stay by 9 days and inpatient cost to over USD 103,860, on top of existing hospital expenses.
Reference
- Heit, John A. “Epidemiology of venous thromboembolism.” Nature reviews. Cardiology vol. 12,8 (2015): 464-74. doi:10.1038/nrcardio.2015.83
- Geerts, William H et al. “Prevention of venous thromboembolism: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines (8th Edition).” Chest vol. 133,6 Suppl (2008): 381S-453S. doi:10.1378/chest.08-0656
- Lin, J et al. “Incremental health care resource utilization and economic burden of venous thromboembolism recurrence from a U.S. payer perspective.” Journal of managed care pharmacy : JMCP vol. 20,2 (2014): 174-86. doi:10.18553/jmcp.2014.20.2.174
- Mahan, Charles E et al. “Venous thromboembolism: annualised United States models for total, hospital-acquired and preventable costs utilising long-term attack rates.” Thrombosis and haemostasis vol. 108,2 (2012): 291-302. doi:10.1160/TH12-03-0162
- Lindblad, B et al. “Incidence of venous thromboembolism verified by necropsy over 30 years.” BMJ (Clinical research ed.) vol. 302,6778 (1991): 709-11. doi:10.1136/bmj.302.6778.709
- Grant, Jonathan D et al. “Diagnosis and management of upper extremity deep-vein thrombosis in adults.” Thrombosis and haemostasis vol. 108,6 (2012): 1097-108. doi:10.1160/TH12-05-0352
- Guyatt, Gordon H et al. “Executive summary: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines.” Chest vol. 141,2 Suppl (2012): 7S-47S. doi:10.1378/chest.1412S3
- Kahn, Susan R. “The post-thrombotic syndrome.” Hematology. American Society of Hematology. Education Program vol. 2016,1 (2016): 413-418. doi:10.1182/asheducation-2016.1.413
- Trivedi, Nikunj N et al. “The Incremental Cost of Inpatient Venous Thromboembolism After Hip Fracture Surgery.” Journal of orthopaedic trauma vol. 34,4 (2020): 169-173. doi:10.1097/BOT.0000000000001675
