3 Main Treatment Strategies for Obstructive Sleep Apnea (OSA)

American Academy of Sleep Medicine (AASM) strongly recommends positive airway pressure for treating OSA in adult patients.
Obstructive sleep apnea (OSA): High Prevalence and Elevated Health Risks The most common type of sleep-disordered breathing, obstructive sleep apnea (OSA), affects over 14% of the global population (1 billion people) 1. Severe sleep disorders raise the patient's risk of all-cause mortality by 3-folds, significantly increasing the chance of chronic and severe health complications and early death.2
Treatment goals for OSA Enhance improvement in daytime symptoms and quality of life, while also improving sleep quality and reducing cardiometabolic risk. Additionally, aim to normalize the apnea-hypopnea index (AHI) and reduce nocturnal oxygen desaturations 3. Effective diagnosis and treatment crucial for individual health and healthcare system burden.
3 main treatment strategies for OSA:
1. Lifestyle Changes
- Weight management and active lifestyle:In the past 5 years, the WHO estimates global obesity to affect almost two billion adults 1. Weight loss and exercise should be recommended to all patients with OSA who are overweight or obese. Exercise may modestly improve OSA even in the absence of significant weight loss 4.
- Quit smoking:Smoke exposure can contribute to airway inflammation, which can narrow the upper airways and predispose to collapse and obstructive apneas 5.
-
Limit alcohol intake:Alcohol can relax the muscles in the back of your throat which can interfere with breathing.
2. Therapies
-
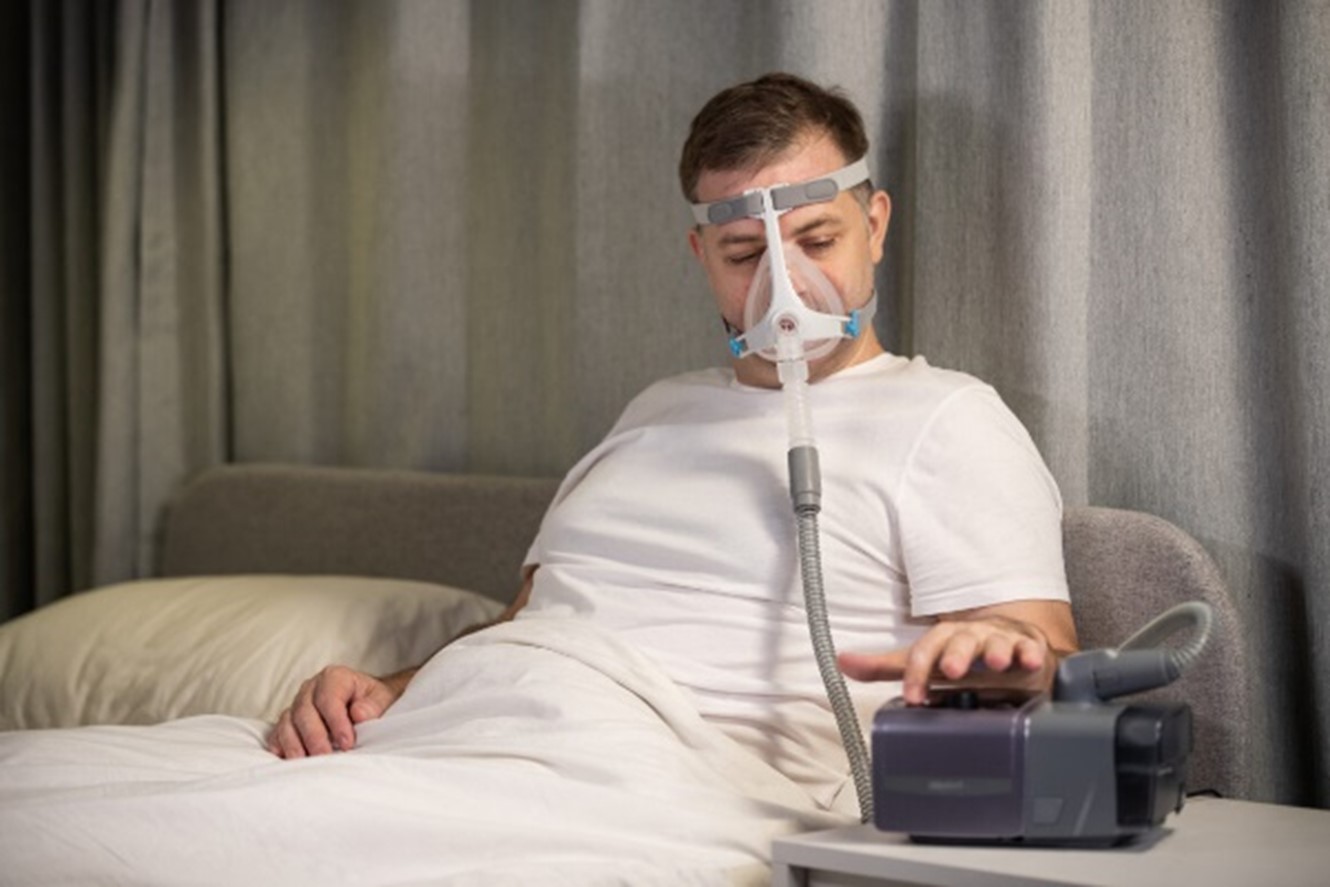
Continuous positive airway pressure (CPAP):American Academy of Sleep Medicine (AASM) strongly recommends positive airway pressure for treating OSA in adult patients4. Respiratory events due to upper airway collapse (eg, apneas, hypopneas) are prevented 5.
- Oral appliance therapy: For patients with mild or moderate OSA who decline or fail to adhere to PAP therapy, an oral appliance is a reasonable alternative to PAP 5.
- Positional therapy (sleep on the side):Sleeping in a non-supine position (eg, lateral recumbent) may correct or improve OSA in such patients and should be encouraged but not generally relied upon as the sole therapy 6.
3. Surgery and other procedures7
- Uvulopalatopharyngoplasty/ UPPP:During this procedure, excess tissue in the throat is removed to widen the airway and allow air to move through the throat more easily.
-
Maxillomandibular advancement:The soft tissues of the airway are also advanced through their attachments to the jawbones, and this leads to a significant expansion of the airway.
"iX series" Solution for Obstructive Sleep Apnea (OSA).
It provides the following benefits for Obstructive Sleep Apnea (OSA) treatment:
1.Automate sleep therapy:
Automatic breathing detection triggers the release of positive pressure immediately after detecting the user's expiration and switches the device to standby mode after brief inactivity, simplifying the therapy process across all levels of users.
2. Digital, Global, and Personal:
Patients can use SleepWell (app) to self-assess therapy effectiveness, while healthcare professionals can utilize SleepWell Track (web) to detect problematic patients and intervene early.
3. Pack-n-Go Sleep Companion:
Travel without the water chamber and switch to regular air tubing for a more straightforward setup, ensuring access to high-quality sleep while travelling small and lightweight.
If want to know about iX series
iX series – Sleep apnea – Respiratory therapy | Wellell
Explore the Impact of Sleep apnea solutions on your hospital
https://www.wellell.com/en/how-can-we-help
#CPAP Therapy#Sleep Apnea Diagnosis#CPAP Equipment#CPAP Machine#Sleep Score Tracking
- Lyons MM, Bhatt NY, Pack AI, Magalang UJ. Global burden of sleep-disordered breathing and its implications. Respirology. 2020 Jul;25(7):690-702. doi: 10.1111/resp.13838. Epub 2020 May 21. PMID: 32436658.
- Young T, Finn L, Peppard PE, Szklo-Coxe M, Austin D, Nieto FJ, Stubbs R, Hla KM. Sleep disordered breathing and mortality: eighteen-year follow-up of the Wisconsin sleep cohort. Sleep. 2008 Aug;31(8):1071-8. PMID: 18714778; PMCID: PMC2542952.
- Mohammadieh, A., Sutherland, K., & Cistulli, P. A. (2017). Sleep disordered breathing: management update. Internal Medicine Journal, 47(11), 1241-1247. doi:10.1111/imj.13606
- Patil SP, Ayappa IA, Caples SM, Kimoff RJ, Patel SR, Harrod CG. Treatment of Adult Obstructive Sleep Apnea with Positive Airway Pressure: An American Academy of Sleep Medicine Clinical Practice Guideline. J Clin Sleep Med. 2019 Feb 15;15(2):335-343. doi: 10.5664/jcsm.7640. PMID: 30736887; PMCID: PMC6374094.
- https://www.uptodate.com/contents/management-of-obstructive-sleep-apnea-in-adults#disclaimerContent
- Krishnan V, Dixon-Williams S, Thornton JD. Where there is smoke…there is sleep apnea: exploring the relationship between smoking and sleep apnea. Chest. 2014 Dec;146(6):1673-1680. doi: 10.1378/chest.14-0772. PMID: 25451354; PMCID: PMC4251622.
- https://www.uofmhealth.org/conditions-treatments/brain-neurological-conditions/surgical-alternatives-cpap

